Persister cells still a problem for Lyme disease patients
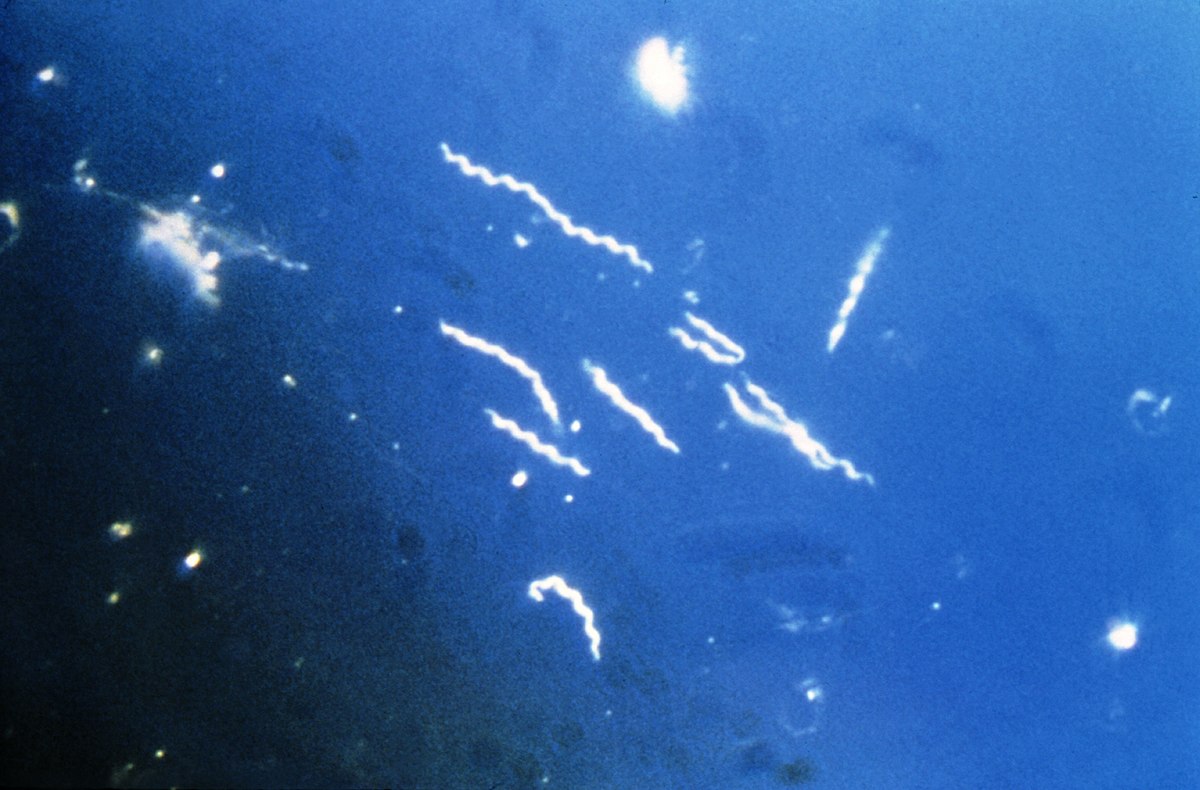
Bacterial persistence is not a new concept. “The term “bacterial persistence” is used to describe the ability of pathogenic bacteria (“persisters”) to survive in infected host tissues despite the presence of effective levels of antimicrobials and antibacterial cellular and humoral immunity,” writes Cabello from New York Medical College in the journal Environmental Microbiology.
There is increasing evidence of bacterial persistence in microbiology. “Though its applicability to B. burgdorferi has been controversial, persistence is a widely-accepted phenomenon in microbiology which in some instances can have therapeutic implications,” according to Cabello. [1]
“While still a matter of dispute, there are numerous reports of antimicrobial treatment unable to completely eliminate B. burgdorferi from the tissues of experimentally infected rodents and nonhuman primates.”
The ability of spirochetes to survive in a tick followed by an animal and back to the tick may explain the persister cell. The metabolic and morphologic changes needed by the spirochete to survive both the tick and vertebrate reservoir may explain “tolerance to otherwise lethal doses of antimicrobials and to other antimicrobial activities,” he points out.
Spirochetes can become tolerant to antimicrobials through phenotypic changes. Phenotypic changes typically involve adaptation to the environment without a genetic change. For example, spirochetes are covered with Outer surface protein A (OspA) in the tick and covered with Outer surface protein C (OspC) in vertebras.
Spirochetes can also adapt in culture. “Stationary phase B. burgdorferi cells in culture can also become phenotypically tolerant to antimicrobials used in treating Lyme borreliosis such as ceftriaxone, doxycycline, and amoxicillin,” according to Cabello.
His examples included, “Readily detectable borrelia tolerant to antimicrobials in suspension cultures and biofilms in vitro, potential refugia for persister spirochetes and apparently quiescent round forms under several kinds of environmental stresses.”
Refugia refers to potentially protected areas for spirochetes. “Borrelia burgdorferi, the tick-transmitted etiologic agent of Lyme borreliosis, can colonize and persist in multiple tissue sites despite vigorous host immune responses,” writes Cabello in his 2007 paper in Trends in Microbiology. [2]
“In infected vertebrate hosts, such refugia could be found in collagenous and other avascular tissues where borrelia are not multiplying.”
The presence of persisters may facilitate emergence of antimicrobial-resistant bacteria. “It should be noted that although persistence is phenotypic, the presence of persisters can also facilitate emergence of genetically antimicrobial-resistant bacteria, e.g., by mutation,” according to Cabello.
References:
- Cabello FC, Godfrey HP, Bugrysheva J, Newman SA. Sleeper cells: The stringent response and persistence in the Borreliella (Borrelia) burgdorferi enzootic cycle. Environ Microbiol. 2017.
- Cabello FC, Godfrey HP, Newman SA. Hidden in plain sight: Borrelia burgdorferi and the extracellular matrix. Trends Microbiol. 2007;15(8):350-354.




R Fanning
07/30/2019 (12:46 pm)
Lyme totally destroys your life. Here in western New York I could not get help from my P C doctor or infectious disease doctors. I went out of state and received help from Lyme literate doctors paying for antibiotic treatment , fuel, hotels, food, and other medications out of pocket, all when I am not working because of this horrific disease. It has been a hard road. The Lyme doctors tell me there is hope of recovery. Progress has been slow. I hope and need to get back to work. If thousands of people are being disabled by this, then how for the love of god ,can doctors and the government continue to misrepresent and ignore this problem with no funding for research.
Karen Austin
01/09/2023 (1:23 pm)
I’m there too R. I’m feeling positive about the new antbitotics that are available now, but thinking I might have to spend my retirement to get rid of this horrible parasite. One friend reminded me of Go Fund Me which could help a bit. Hope you are Lyme free!
bonnie
11/02/2018 (8:04 pm)
what is effective at treating persisters?
Dr. Daniel Cameron
11/05/2018 (9:21 am)
The video highlights the work in the lab. Some of the treatments in the labs are not available yet on the market. Dapsone is on the market but it benefit are risks have not been worked out.