Anaplasmosis associated with cardiac complications
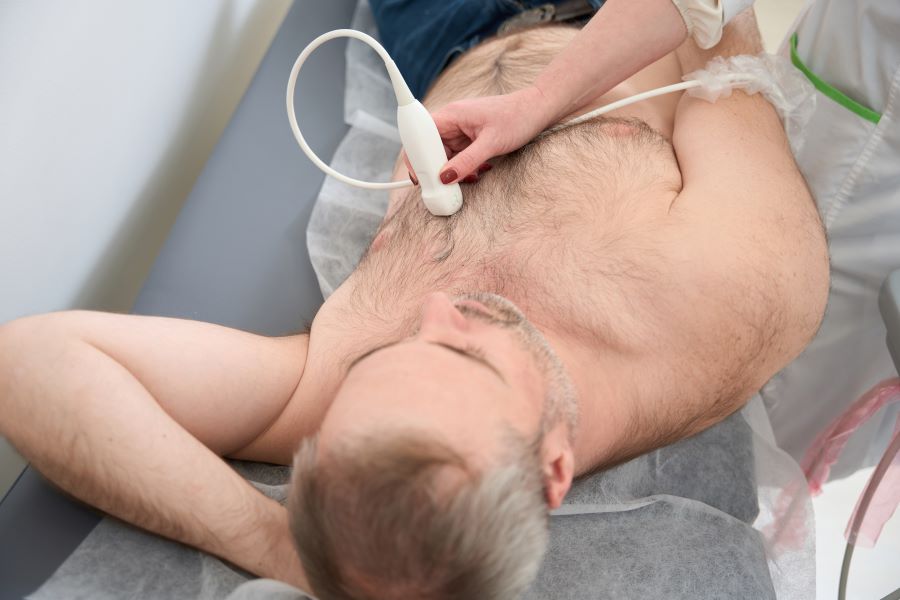
There have only been a few reported cases of myocarditis occurring in individuals with anaplasmosis. In a recent study, investigators describe a 61-year-old man who was diagnosed with myopericarditis related to anaplasmosis. The patient also tested positive for Lyme disease.
Acute Lyme disease causes complete heart block
Carditis is a rare complication of Lyme disease and usually occurs several weeks after exposure to a tick bite. Conduction abnormalities are the most common manifestation of Lyme carditis.
Lyme neuroborreliosis mimics Guillain-Barré Syndrome
Guillain-Barré Syndrome (GBS) is an autoimmune disorder which involves your immune system mistakenly attacking the peripheral nerves outside of the brain and spinal cord. It typically presents with weakness and/or tingling sensations in the legs, which can progress and spread to the arms and upper body.
Borrelia burgdorferi causes prosthetic joint infection
In their case report “Borrelia burgdorferi—A Bacterium Worthy of Consideration in Culture-Negative Prosthetic Joint Infection,” Crowe and colleagues describe a patient who developed a prosthetic joint infection due to Borrelia burgdorferi. [1]
Anaplasma phagocytophilum infection triggers encephalitis
Anaplasmosis rarely causes neurologic complications. But the authors of a new study, describe a patient who developed encephalitis due to an infection with Anaplasma phagocytophilum. This is believed to be the first case reported in the literature of Anaplasma encephalitis.
Autism (ASD) symptoms improve following treatment for Lyme disease
In their case report, investigators describe a child with autism spectrum disorder (ASD), whose cognitive and neuropsychiatric symptoms resolved completely or improved substantially after he was treated with antibiotics for Lyme disease and Bartonella.
4 cases of Powassan virus encephalitis
Powassan virus (POWV) can cause a rare but potentially life-threatening disease including encephalitis. In this case review, the authors describe 4 patients with Powassan virus encephalitis, who were all treated at a hospital in North Dakota. The patients resided in North Dakota and Wisconsin.
Pregnancy, breast feeding and Lyme
Children with Lyme disease can suffer both academically and physically. Neurological, psychiatric, and cognitive symptoms can drastically impair an ability to learn and grow in the classroom. In addition, adolescents may struggle socially, unable to connect with their peers or participate, as they once could, in extracurricular activities.
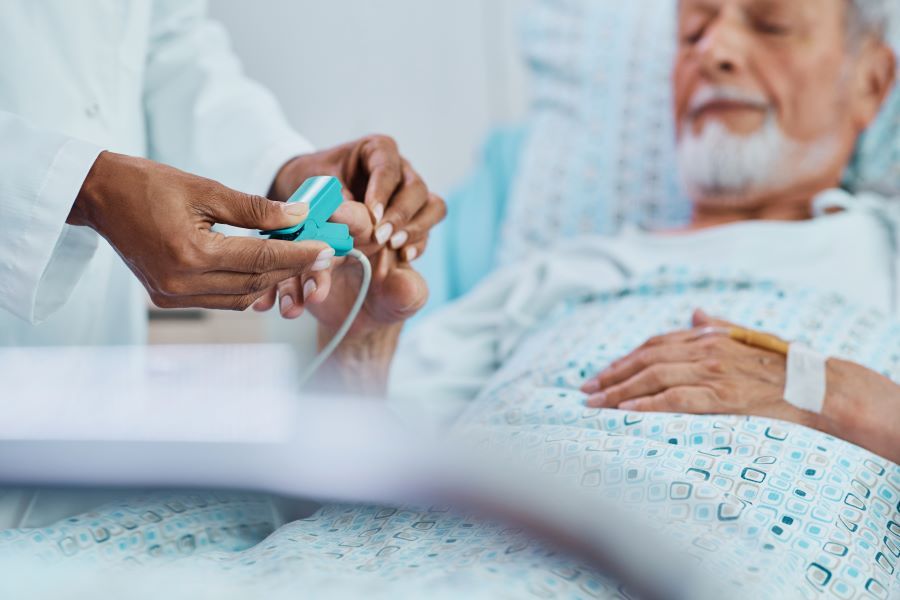
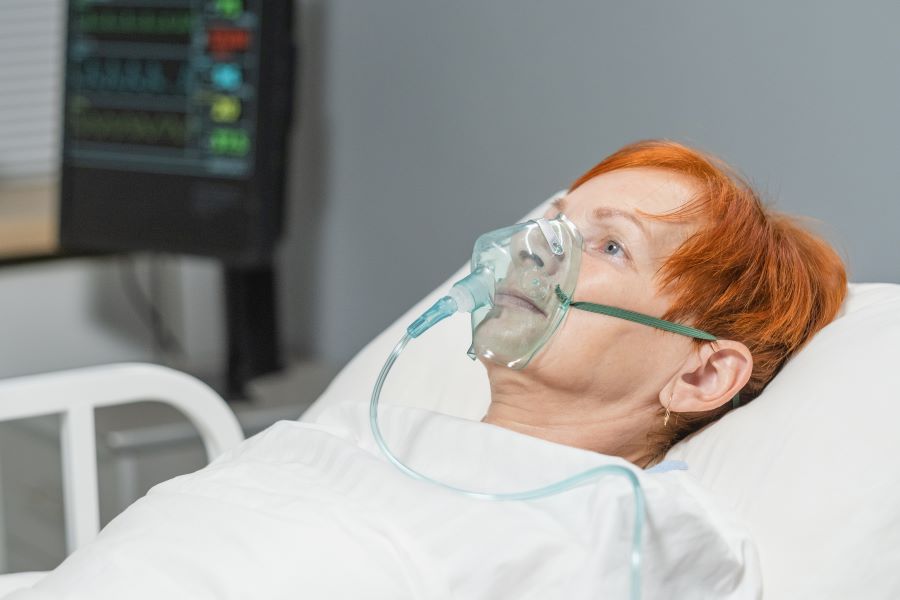
Severe anaplasmosis leads to multi-organ complications
Anaplasmosis can present with a wide range of symptoms, making it challenging to diagnose. The most common symptoms include fever, headache, muscle aches, fatigue, and chills. However, in severe cases, anaplasmosis can affect multiple organ systems, causing respiratory failure, kidney failure, and bleeding disorders. In rare cases, it can be fatal.
Disturbed hearing, sleep, and smell in Lyme
Welcome to another selection from my book "An Expert's Guide on Navigating Lyme disease." The book highlights the findings of my first 600 Lyme disease Science blogs. In this episode, I will discuss disturbed hearing, sleep, and smell in Lyme.
By Dr. Daniel Cameron
Lyme disease can lead to disturbed hearing, sleep, and smell.
Lyme disease associated with hearing loss and tinnitus.
The majority of patients with tick-borne diseases admitted to an outpatient otolaryngologic clinic in Poland suffered from hearing loss and tinnitus.
The most common complaint ...