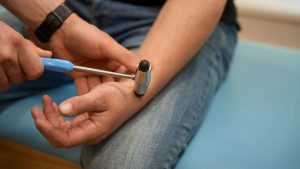
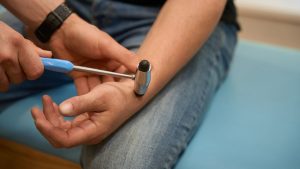
Chronic Lyme Disease Misdiagnosis: When Occam’s Razor Fails
In medicine, Occam’s razor teaches that the simplest explanation is often the right one. But chronic Lyme disease misdiagnosis often reflects a deeper problem: the simplest explanation may be overlooked. In chronic Lyme, this idea is sometimes used against patients. Ongoing symptoms are too quickly explained away with theories that do not fit the real clinical picture. The simplest answer—that the infection may not have been fully cleared—deserves more careful attention.
For a broader look at why Lyme disease challenges conventional diagnostic thinking, see Why Lyme Disease Tests the Limits of Medicine.
Chronic Lyme Disease Misdiagnosis: The “Alternative Explanations” Patients Hear
Instead of recognizing that chronic Lyme symptoms may come from a lingering infection, patients are often told their struggles are due to stress, depression, anxiety, or other unrelated conditions. Patients may be told symptoms are due to:
- “Immune debris” — lingering bacterial fragments
- “Post-infectious inflammation” — immune activation after infection
- Central sensitization — the nervous system becomes overly sensitive and keeps amplifying pain signals, even after the original illness has healed
- Autoimmune reactions without infection — the body attacking its own tissues
- Functional diagnoses — fibromyalgia or chronic fatigue syndrome
- Psychological factors — stress, anxiety, or trauma
Some patients receive the label post-treatment Lyme disease syndrome (PTLDS). But using these explanations too quickly can contribute to chronic Lyme disease misdiagnosis by shifting attention away from persistent infection and co-infections that still deserve careful clinical review.
In the context of chronic Lyme, invoking Occam’s razor should not shut down the conversation. Instead, it should prompt a thoughtful review for persistent infection and possible co-infections so patients get the answers and care they need.
Why Ignoring Persistent Infection Breaks Occam’s Razor
Multiple factors can exist, but dismissing infection in favor of more abstract explanations can actually violate Occam’s razor. In chronic Lyme, overlooking a persistent Borrelia infection or co-infection can turn a clear unifying explanation into unnecessary complexity.
This is where theory meets clinical reality.
Persistent Infection: The Signs
Patients often present with symptoms consistent with active disease, including:
- Cognitive slowing and memory problems
- Sensory hypersensitivity
- Impaired balance or coordination
- Crushing fatigue
- Migratory joint or nerve pain
- Autonomic symptoms, such as rapid heart rate or dizziness
These symptoms often fit more closely with an active infection than with unrelated explanations such as “leftover debris.” Avoiding chronic Lyme disease misdiagnosis requires clinicians to consider whether infection is still driving the illness.
In chronic Lyme, the simplest explanation is often the most overlooked: the infection may still be active.
The Risks of Getting Occam’s Razor Wrong
Misapplying Occam’s razor in chronic Lyme cases can lead to:
- Missed diagnosis of persistent Borrelia or other tick-borne pathogens
- Delayed treatment and irreversible damage
- Loss of years of potential recovery
- Declining quality of life and disability
A Smarter Diagnostic Approach
Occam’s razor is a useful tool when applied correctly. In chronic Lyme, that means ruling out persistent infection before accepting more complex theories. A common driver of chronic Lyme disease misdiagnosis is the premature assumption that infection is no longer relevant.
Hickam’s dictum, the counterpoint to Occam’s razor, reminds us that patients can have more than one problem at once. Co-infections, immune dysfunction, autonomic dysfunction, and secondary complications can coexist with infection rather than replace it.
The Takeaway:
When applied to chronic Lyme disease, Occam’s razor should point toward the simplest unifying cause: persistent infection. Ignoring that possibility risks missing the diagnosis that matters most.
Resources:
Dr. Daniel Cameron, MD, MPH
Lyme disease clinician with over 30 years of experience and past president of ILADS.
Symptoms • Testing • Coinfections • Recovery • Pediatric • Prevention