
The Ethics of Lyme Disease Treatment: Patient Rights and Physician Responsibility
The ethics of Lyme disease treatment often arise at the intersection of diagnostic uncertainty, guideline interpretation, and patient suffering. Lyme disease does not always follow predictable timelines. When symptoms persist or testing does not align neatly with clinical presentation, ethical tension can emerge.
Ethical care requires more than protocol alone. It requires disciplined reasoning, intellectual humility, and the willingness to reassess when patients do not follow expected trajectories.
In complex illness, ethical decision-making is rarely about choosing between right and wrong. More often, it involves navigating uncertainty while protecting patient safety and dignity.
Where Ethical Tension Arises
Ethical challenges frequently emerge when clinical guidelines intersect with individual variability. Standardized recommendations provide structure, yet no guideline can account for every biologic difference or clinical presentation.
When a patient’s symptoms persist despite standard therapy, clinicians face a difficult question: Does continued evaluation represent appropriate reassessment, or unnecessary deviation from protocol?
The ethical obligation is not blind adherence nor reflexive escalation. It is careful clinical reasoning grounded in evidence, experience, and patient-centered evaluation.
Diagnostic Uncertainty and Responsibility
Lyme disease testing has known limitations. Antibody-based tests may be negative early in infection or may not fully capture complex presentations. Ethical practice requires acknowledging these limitations openly rather than overstating diagnostic certainty.
Premature diagnostic closure — stopping investigation once a plausible explanation appears — can unintentionally contribute to patient harm. Recognizing cognitive bias is part of ethical clinical maturity.
Uncertainty is uncomfortable. Yet ethical care often requires tolerating uncertainty while continuing disciplined reassessment.
Balancing Guidelines and Individual Care
Clinical guidelines are designed to standardize care across populations. Ethical practice requires applying them thoughtfully rather than rigidly.
- Assess individual risk factors and exposure history
- Reevaluate when symptom evolution does not match expectations
- Consider co-infections or overlapping syndromes
- Recognize testing limitations
- Maintain longitudinal follow-up when appropriate
The goal is not to reject evidence-based medicine. The goal is to apply it with clinical judgment and flexibility.
Respecting Patient Experience
Ethical care includes listening carefully to patient-reported symptoms. Persistent fatigue, cognitive dysfunction, pain, and autonomic symptoms may not always fit simplified models of acute infection.
Listening does not require immediate agreement with every hypothesis. It requires maintaining curiosity rather than narrowing inquiry prematurely.
When patients feel unheard, trust erodes. Ethical practice protects that trust.
Clinical Takeaway
The ethics of Lyme disease treatment demand disciplined reasoning, humility in the face of uncertainty, and commitment to patient-centered care. Guidelines provide structure. Clinical experience provides context. Ethical maturity lies in balancing both.
In complex illness, humility is protective. Curiosity prevents harm.
About the Author
Reviewed and authored by Daniel Cameron, MD, MPH
Dr. Cameron is a board-certified physician with over 37 years of clinical experience treating Lyme disease and tick-borne illnesses. A past president of the International Lyme and Associated Diseases Society (ILADS), he has contributed to national discussions on diagnostic limitations, medical ethics, and complex patient care.
This article reflects his clinical experience and review of current research.
Dr. Daniel Cameron, MD, MPH
Lyme disease clinician with over 30 years of experience and past president of ILADS.
Symptoms • Testing • Coinfections • Recovery • Pediatric • Prevention
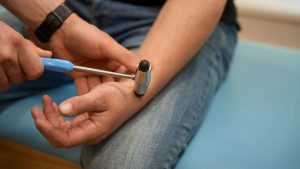
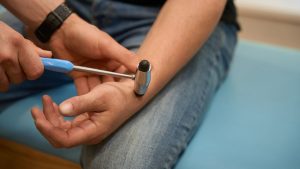

In regard to your FAQ,s above (#1), why will you not move beyond ILADS treatment protocols and treat me with the Dapsone protocol that has shown to be effective with years long remissions? Have you forgotten that you once started with experimentation on patients 37 years ago to arrive at your published protocols that are good, but do not work for all patients?
I understand the frustration behind this question. Lyme disease can be complex, and not every approach works for every patient. My treatment decisions are guided by patient safety, clinical experience, and the best available evidence at this time. I continue to follow the research as it evolves.
As the saying goes, “nurse, heal thyself”. And I will, I have the means to do so. Too bad I have to go it alone.