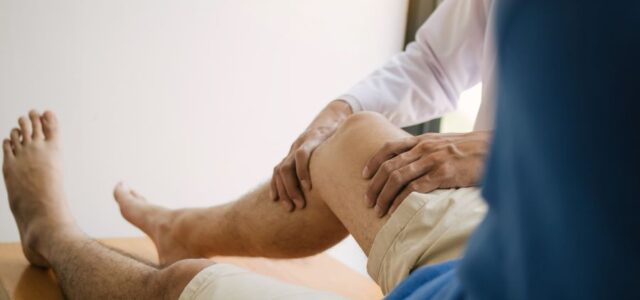
MRI Helps Identify Lyme Arthritis, Avoid Child Surgery
Fourteen children underwent knee surgery for what doctors thought was septic arthritis—but all 14 actually had Lyme disease. Yen and colleagues examined whether MRI imaging could have prevented these unnecessary surgical procedures in pediatric patients with acute knee effusion.
The study reviewed medical records and MRI scans of 87 children with Lyme arthritis and 9 with septic arthritis. The findings reveal a diagnostic gap that affects 16% of pediatric Lyme arthritis cases in endemic areas.
For a broader discussion of why Lyme disease is frequently overlooked in children, see Pediatric Lyme Disease: Why Children Are Often Misdiagnosed.
Lyme Arthritis vs Septic Arthritis: Key Study Findings
The study examined 96 children total:
- 87 cases confirmed as Lyme arthritis (91%)
- 9 cases confirmed as septic arthritis (9%)
- 14 Lyme arthritis patients (16%) underwent unnecessary surgery
- 100% of Lyme arthritis patients responded to 1 month of oral antibiotics
- 0 Lyme arthritis patients required surgical drainage after correct diagnosis
These numbers highlight the diagnostic challenge facing clinicians in endemic areas and the potential impact of improved diagnostic protocols.
Why Lyme Arthritis Gets Mistaken for Septic Arthritis
Patients with Lyme arthritis can exhibit fever, inability to bear weight, elevated CRP and ESR, and high synovial white blood cell count from an arthrocentesis. These findings can mimic bacterial septic arthritis.
However, the arthritis caused by the Borrelia burgdorferi spirochete is distinct from bacterial septic arthritis. Lyme arthritis does not cause the rapid articular cartilage destruction seen in septic arthritis and therefore does not typically require emergency surgical drainage.
This distinction matters clinically and financially. Fourteen patients in this study underwent unnecessary surgical procedures based on the presumption of septic arthritis.
MRI Findings That Predict Lyme Arthritis
The study identified specific MRI and clinical criteria that can predict Lyme arthritis and help avoid surgery. Patients with lymphadenopathy, myositis, and CRP of less than 3 mg/L—without subcutaneous edema—who are able to bear weight can be treated with oral antibiotics for Lyme arthritis while awaiting serologic results.
MRI findings can indicate septic joints in as little as 24 hours after infection. The imaging modality has proven extremely effective in evaluating musculoskeletal infections.
The authors offer a useful prediction algorithm for Lyme arthritis that includes MRI for the evaluation of patients presenting with acute inflammation of the knee. Had these criteria been applied to the 14 patients who underwent surgery, all may have avoided the surgical procedure.
MRI Considerations in Pediatric Practice
Testing with MRI can be costly and may require sedation for some young patients. However, the diagnostic accuracy and potential to avoid unnecessary surgery may justify these costs and risks.
All 87 Lyme arthritis patients in this study were treated with 1 month of antibiotics. The addition of MRI criteria to clinical and laboratory findings significantly improved the predictive value for identifying Lyme arthritis.
Clinical Implications for Lyme-Endemic Areas
Lyme arthritis should be strongly suspected in endemic areas of the United States when children present with a knee effusion. The combination of clinical presentation, laboratory values, and MRI findings can guide treatment decisions.
The addition of MRI criteria to clinical and laboratory findings significantly improved the predictive value for identifying Lyme arthritis. This approach can prevent both unnecessary surgery and the complications associated with delayed antibiotic treatment.
When Parents Should Ask About MRI for Knee Swelling
If your child presents with knee swelling in a Lyme-endemic area, consider requesting MRI evaluation when:
- Your child can still bear weight despite the swelling
- There is no significant subcutaneous edema (swelling under the skin)
- Your child has been outdoors in areas where tick exposure is possible
- Laboratory testing shows CRP less than 3 mg/L
- Surgery is being recommended based on presumed septic arthritis
MRI can provide critical information before proceeding to surgical intervention. While the test may require sedation for young children, it can prevent unnecessary operative procedures.
Frequently Asked Questions
How can doctors tell the difference between Lyme arthritis and septic arthritis in children?
MRI findings combined with clinical criteria can help distinguish the two conditions. Patients with Lyme arthritis often show lymphadenopathy, myositis, CRP less than 3 mg/L, no subcutaneous edema, and ability to bear weight—features that differ from septic arthritis patterns on imaging and examination.
Why is it important to distinguish Lyme arthritis from septic arthritis?
Lyme arthritis does not cause the rapid cartilage destruction seen in septic arthritis and does not require emergency surgical drainage. This study found that 16% of Lyme arthritis patients underwent unnecessary surgery because they were initially presumed to have septic arthritis.
Does my child need surgery for Lyme arthritis?
No. Lyme arthritis does not require surgical drainage and responds to antibiotic treatment. This study found that all 87 children with Lyme arthritis were successfully treated with 1 month of oral antibiotics alone. Surgery should only be considered if septic arthritis is confirmed, not presumed.
What is the treatment for Lyme arthritis in children?
All Lyme arthritis patients in this study were treated with 1 month of oral antibiotics. Patients meeting specific MRI and clinical criteria can begin antibiotic treatment while awaiting serologic confirmation, avoiding the need for surgical drainage.
When should doctors suspect Lyme arthritis in children with knee swelling?
Lyme arthritis should be strongly suspected in Lyme-endemic areas when children present with knee effusion, especially when MRI shows lymphadenopathy and myositis, CRP is less than 3 mg/L, there is no subcutaneous edema, and the child can bear weight.
Related Reading
- Pediatric Lyme Disease: Why Children Are Often Misdiagnosed
- Lyme Arthritis Symptoms in Child Years After Tick Bite
- Diagnosing Lyme Arthritis of the Hip in Children
- High Cost of Treating Lyme Arthritis in Children with Surgery
References
- Yen YM, Sanborn RM, Donohue K, Miller PE, Milewski MD, Ecklund K. Lyme Arthritis in the Pediatric Knee: Clinical and Magnetic Resonance Imaging Differentiators. JB JS Open Access. 2022 Nov 23;7(4):e22.00067.
Dr. Daniel Cameron, MD, MPH
Lyme disease clinician with over 30 years of experience and past president of ILADS.
Symptoms • Testing • Coinfections • Recovery • Pediatric • Prevention


I’m confused by this article. Isn’t septic arthritis most usually bacterial related? And couldn’t the septic arthritis patients been Lyme ( or go infection) related but not caught in western blot etc (due to immune deficits/imbalances as a result of Borrelia occupying immune cells) ? Wouldn’t it be prudent to always test a sample of synovial fluid to determine the presence and type infection, ( particularly using dark field microscope), since other bacteria such as bartonella reportedly can also cause arthritis? MRI can cause mast cell reactions in some people ( at least in a observational sample of persons carrying HaTS trait ) ; besides being much more expensive than a simple surgical aspiration of fluid that can be fine in a doctors office. Is this the surgical procedure they refer to? Or were kids operated on in more invasive procedures. Didn’t quite get the definition of surgical in the article; maybe yes he, but the article is confusing to me. Thanks! Angela BK
There are different definitions for Septic arthritis. The cause can be bacterial, viral, and fungal. The most famous but uncommon are staph infections.