Call for your appointment today 914-666-4665 | Mt. Kisco, New York

by Daniel J. Cameron, MD MPH
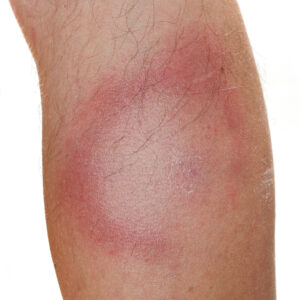
In the Archives of Clinical Neuropsychology, the authors report a substantial number of patients who suffered from severe fatigue, pain and Post-Treatment Lyme disease Syndrome (PTLDS) six months after completing a three-week course of antibiotics for an erythema migrans rash. [4] Out of 107 patients, 6 of the 107 patients (6%) had PTLDS.
The authors suggested, “patients with symptoms of pain, fatigue, and depression on standardized instruments can be referred for appropriate behavioral and medicinal interventions to reduce the impact of these symptoms on daily life functioning.” Bechtold added, “If there is sufficient concern after education and interventions have been applied, then patients can be referred for neuropsychological evaluation.”
Re-treatment with antibiotics should be considered when symptoms persist. “Studies using rodent and primate models have suggested that the persistence of bacteria and/or spirochetal antigens after antibiotic therapy may drive disease,” according to Aucott from Johns Hopkins University School of Medicine. [5] “The use of short-term antibiotic retreatment in the early, post-treatment phase of Lyme disease has yet to be formally tested, although it may be widely applied in clinical practice.”
In fact, Bechtold and colleagues were able to identify 8 cases for early re-treatment. “Of the 107 cases, eight cases were re-treated with antibiotics after the initial 3-week course of doxycycline because there was development of new objective findings (e.g., new neuropathy; five cases) or the EM rash did not fade after initial treatment or new rashes developed in other areas of the body (three cases),” according to Bechtold. [4] Only 2 of the 6 PTLDS patients were re-treated. Most of the cases with severe fatigue and pain were not re-treated.
References:
- Logigian EL, Kaplan RF, Steere AC. Chronic neurologic manifestations of Lyme disease. N Engl J Med. 1990;323(21):1438-1444.
- Klempner MS, Hu LT, Evans J, et al. Two controlled trials of antibiotic treatment in patients with persistent symptoms and a history of Lyme disease. N Engl J Med. 2001;345(2):85-92.
- Fallon BA, Keilp JG, Corbera KM, et al. A randomized, placebo-controlled trial of repeated IV antibiotic therapy for Lyme encephalopathy. Neurology. 2008;70(13):992-1003.
- Bechtold KT, Rebman AW, Crowder LA, Johnson-Greene D, Aucott JN. Standardized Symptom Measurement of Individuals with Early Lyme Disease Over Time. Arch Clin Neuropsychol. 2017;32(2):129-141.
- Aucott JN, Soloski MJ, Rebman AW, et al. CCL19 as a Chemokine Risk Factor for Post-Treatment Lyme Disease Syndrome: A Prospective Clinical Cohort Study. Clin Vaccine Immunol. 2016.




Why is it not recognized by most Dr’s? I googled for a Dr here in WV and out of 20 listested, all but 3 were psychiatrists? I was need Dr taken seriously at ER or Dr’s and never given antibiotics. Now I am bed ridden. Would give anything to be tested correctly. I have found black specks coming put of my skin using coconut oil, or peroxide, also small sperm shaped things in mouth after eating cherry popcycle, put samples in alcohol to preserve, coughed up fluke looking things, thrown up worms after ingesting turpentine and found worms in mucous from bowls. I have hard scabs all over head that are clear and red spots, when pick them off, if I am able to pry up, there’s black specks and hard salt like things. I have crusted scabs on my face and body I can’t get rid of. The rx I was given for cream costs 9000. This is insane and ruining my life…..
It can be difficult to find a diagnosis. There are a growing number of conditions that are yet to be explained even in the tick borne illnesses. Morgellon’s includes a rash but the etiology remains unknown. There are people with Morgellon’s who also have Lyme disease.