Lyme Disease Symptoms That Mimic Chikungunya
Lyme disease and chikungunya may share fatigue, rash, fever, and joint pain
Mosquito-borne and tick-borne illnesses can overlap clinically
Persistent symptoms may complicate diagnosis
The Chikungunya virus (CHIKV) can cause flu-like symptoms, including fevers, headaches, joint pain, muscle aches, nausea, rashes, and malaise. Many of these symptoms overlap with Lyme disease, making diagnosis more challenging when patients present with persistent fatigue, pain, or neurologic complaints.
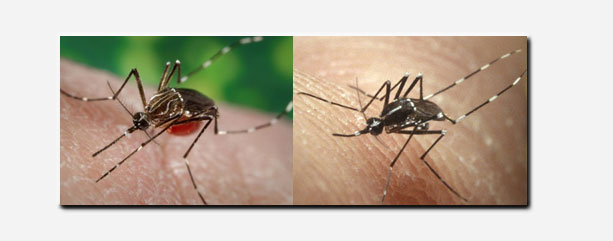
CHIKV symptoms typically develop 3 to 5 days after a person is bitten by an infected mosquito. The two mosquito species most commonly associated with chikungunya transmission are Aedes aegypti and Aedes albopictus.
Although Lyme disease is transmitted by infected blacklegged ticks rather than mosquitoes, the overlap in symptoms may lead to diagnostic confusion, particularly in patients presenting with diffuse musculoskeletal complaints, headaches, fatigue, or chronic arthritic symptoms.
Chikungunya symptoms may persist for months or even years in some individuals. Chronic joint pain and inflammatory arthritis after chikungunya infection can resemble both rheumatoid arthritis and Lyme disease.
According to the Pan American Health Organization, most patients recover fully, but some experience prolonged joint pain and disability. Similar concerns arise in Lyme disease patients with persistent symptoms following delayed diagnosis or treatment.
Researchers have also warned that chikungunya-associated arthritis may mimic seronegative rheumatoid arthritis. In one study published in Arthritis and Rheumatology, patients developed persistent symmetric polyarthritis after travel-associated CHIKV infection.
The affected patients reported morning stiffness and chronic arthritis involving the wrists, hands, ankles, and feet. Some experienced difficulty walking because of severe ankle and foot pain. Similar symptom patterns may also be seen in Lyme disease.
As global vector-borne illnesses expand, clinicians may increasingly encounter patients whose symptoms overlap across multiple infectious diseases. Fever, rash, fatigue, headache, joint pain, and cognitive complaints may occur in both mosquito-borne and tick-borne illnesses.
Physicians evaluating chronic arthritic symptoms should consider a broad differential diagnosis that includes chikungunya, Lyme disease, autoimmune disease, and other vector-borne infections.
Frequently Asked Questions
Can Lyme disease symptoms mimic chikungunya?
Yes. Lyme disease and chikungunya may both cause fatigue, fever, headaches, rash, muscle pain, and joint pain. Chronic arthritic symptoms can overlap significantly.
Can mosquitoes carry Lyme disease?
No. Lyme disease is primarily transmitted through infected blacklegged ticks, not mosquitoes. However, mosquito-borne infections such as chikungunya can cause symptoms that resemble Lyme disease.
What symptoms overlap between chikungunya and Lyme disease?
Both illnesses may present with fatigue, headaches, rash, muscle aches, joint pain, and difficulty with concentration or daily functioning.
Can chikungunya cause chronic arthritis?
Yes. Some patients with chikungunya develop persistent inflammatory joint symptoms lasting months or years after the initial infection.
Why is accurate diagnosis important?
Different vector-borne diseases may require different testing approaches, monitoring strategies, and treatment plans. Persistent symptoms should prompt careful clinical evaluation.
Clinical Takeaway
Chikungunya and Lyme disease illustrate how vector-borne illnesses can produce overlapping symptom patterns that complicate diagnosis. Persistent joint pain, fatigue, headaches, and cognitive complaints may occur in both conditions, increasing the risk of delayed recognition.
As mosquito-borne and tick-borne diseases continue to expand geographically, clinicians may need to consider broader infectious differentials when evaluating patients with chronic inflammatory or neurologic symptoms.
Related Articles
Lyme disease symptoms guide
What can mimic Lyme disease?
Lyme disease misdiagnosis
Delayed Lyme disease diagnosis
Diseases from ticks
References
- Miner JJ, Aw-Yeang HX, Fox JM, et al. Chikungunya viral arthritis in the United States: a mimic of seronegative rheumatoid arthritis. Arthritis Rheumatol. 2015;67(5):1214-1220.
- Pan American Health Organization. Chikungunya fact sheet.
- Staples JE, Fischer M. Chikungunya virus in the Americas — what a vectorborne pathogen can do. N Engl J Med. 2014;371(10):887-889.
Dr. Daniel Cameron, MD, MPH
Lyme disease clinician with over 30 years of experience and past president of ILADS.
Symptoms • Testing • Coinfections • Recovery • Pediatric • Prevention


Had tick bite may or june 2014. Immediate onset total left side numbness nov 2014. Dec 10 right side overnite onset.numbness that is now terrible pain…blood tider and LP negative. MASSIVE pain and numbness extreme pain.Doctors and Neurologists baffled …Refuse to treat for lyme or possible tick born disease. All test show no loss of strength.I’m breaking and cannot tolerate. Somebody please help. I am on YouTube with 590,000 but now hands are so stiff I can’t play…I must get help or its the end I greatly fear. Somebody please contact me with guidance and helpme get appointment with infectious disease Dr.I’m in Kernersville NC
A relative was previously very healthy – perhaps exceptionally healthy. She was bitten by a chikungunya infected mosquito in October and has been afflicted ever since.
Have there been any advances in treatment since you wrote this? Where is the hotbed for research in the US (or world) for chikungunya?
Thanks for your work with Lyme patients. I’ve referred many friends and strangers to you even though I’ve never been your patient. I should have been. I had the classic Lyme bullseye as far back as the mid 70s after a tick bite.
Thanks for your continued work transforming lives.
I have not heard of any breakthroughs on the chikungunya virus. It always harder to treat a virus. It is also important not to overlook another illness including a tick borne illness if symptoms persist.
My 10 yr old daughter has been sick for 3 months and Drs are baffled at what it is. It started with pain all over, stiff neck, joint pain and extreme fatigue. A simple bath wears her out! She had mono 3 years ago but has tested negative for active infection now. They tested for Lyme and got a positive result but negative antibodies test. So Drs say we got a false positive. She says the pain is getting worse and is worse than when she had mono. Is this something Dr.’s would normally test for or do I need to ask for this specific test for chikungunya . Thank you in advance for any insight. It’s awful to watch your child in pain and not know why.
Sorry to hear your daughter remains ill. The blog reflects the difficulties doctors can have telling the difference between even the Chikungunya virus and Lyme disease. It would be reasonable to look a second time at Lyme disease given the limitations of the testing.
Thank you so much Dr. Cameron I will ask for them to test again.
After spending a week in Arkansas at a remote lake I came home with what seems like mosquito bites. After being home for one day it appears that I have slept for 20+ hours and I am extremely tired and have some dizziness. Is there a reason that I should seek medical help?
I would advise a medical evaluation that includes tick borne illnesses.
I’ve had pain and swelling since May 2016 that followed nearly a year of flulike symptoms – fever, fatigue, sore throat, cough, dizziness, loss of taste/smell – and had swollen lymph nodes. The pain started on my dominant hand’s index finger that spread to my hand after 3 months.
In 2019, it spread to the other hand and work/hobbies became impossible, even holding a fork, pinching food, and turning door knobs is difficult. Now it’s in both my feet as well and I am steps away from being truly unable to live independently without any answers as all of my imaging and blood tests are coming back normal.
Should I pursue further investigation for Lyme? Should I ask about CHIKV? I’m 24, eat a healthy diet (as anything unhealthy triggers inflammation and increases aching in my hands and feet), try to at least exercise as regularly as possible (as that’s the least hobby standing), and I’m worried that if I go for a walk outside or go on a long drive, I won’t be able to make it home.
I advise my patients with these issues to include an evaluation for a tick borne infection as part of their overall care. I don’t typically see CHIKV in my practice.