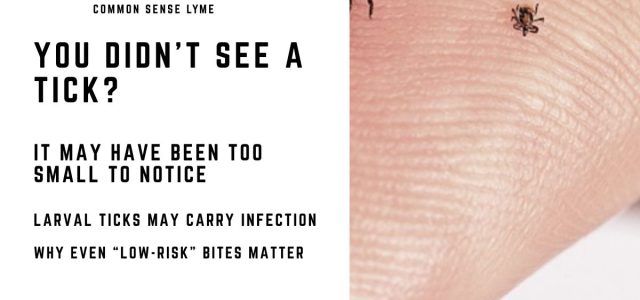
Can Larval Ticks Spread Disease? Borrelia Miyamotoi Risk Explained
Can larval ticks spread disease? Emerging research suggests they can—and the risk may be higher than previously believed.
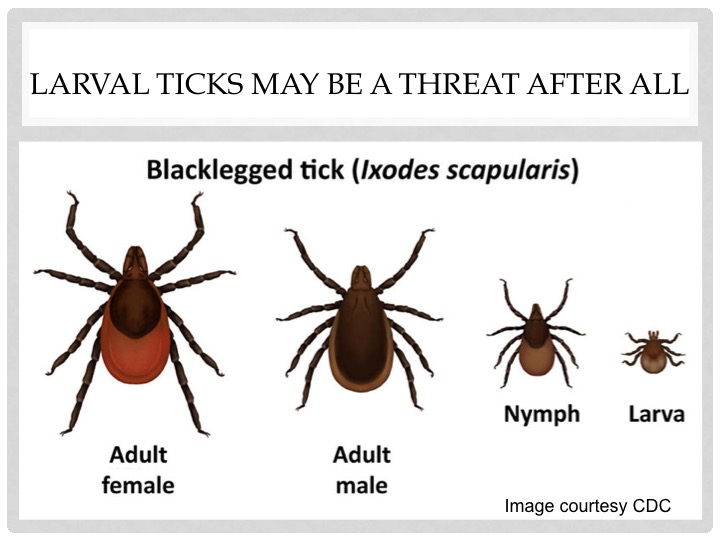
For years, nymphal ticks have been considered the primary source of tick-borne infections. But new evidence indicates that larval ticks—despite their microscopic size—may also transmit infections such as Borrelia miyamotoi.
Quick answer: Larval ticks may carry infection from birth and transmit disease during their first blood meal, making them a potential but often overlooked source of exposure.
For a broader overview, see Lyme disease symptoms guide.
Why Larval Ticks May Transmit Infection
Larval ticks hatch from eggs with six legs and are extremely small—often difficult to detect on the skin.
Traditionally, they were not considered a major health threat because they were thought to acquire infection only after feeding.
However, newer research suggests that some pathogens, including Borrelia miyamotoi, may be transmitted from the adult female tick directly to her offspring.
This means larval ticks may already be infected before their first bite.
Seasonal Patterns Suggest Larval Transmission
Clinical observations support this concern.
In case series of Borrelia miyamotoi disease, most infections occurred in July and August—when larval ticks are most active.
This differs from Lyme disease, which typically peaks earlier during nymph season.
The timing raises the possibility that larval ticks are contributing to transmission.
Why Larval Tick Bites Are Easy to Miss
Larval ticks are smaller than a poppy seed and often go completely unnoticed.
Like other ticks, they can:
- Attach in hidden areas such as the scalp or behind the knees
- Inject anesthetic compounds that prevent pain
- Remain undetected during routine tick checks
This makes them a potential hidden source of infection.
Symptoms of Borrelia Miyamotoi Infection
Borrelia miyamotoi disease often presents as a nonspecific febrile illness.
Common symptoms include:
- Fever
- Fatigue
- Headache
- Muscle aches
Laboratory findings may include:
- Abnormal liver enzymes
- Leukopenia
- Thrombocytopenia
Unlike Lyme disease, rash is typically absent.
Diagnostic Challenges
Diagnosis can be difficult.
Testing for Borrelia miyamotoi is not widely available, and symptoms often overlap with other tick-borne illnesses.
Clinical judgment is essential—especially in patients with summer fever and no clear diagnosis.
Overlap with Lyme Disease and Co-Infections
Patients with suspected Lyme disease may actually have:
- Borrelia burgdorferi
- Borrelia miyamotoi
- Or both infections
This overlap can complicate diagnosis and delay appropriate treatment.
Learn more about Lyme disease co-infections.
Treatment Considerations
Current treatment recommendations are based on limited data.
Reported effective therapies include:
- Doxycycline and other tetracyclines
- Amoxicillin
- Cefuroxime
- Azithromycin (presumed effective)
Long-term outcomes remain uncertain, as most studies focus on acute infection.
Clinical Perspective and Takeaway
If larval ticks can transmit infection, current assumptions about tick risk may need to change.
Larval ticks may be an underrecognized source of tick-borne infection.
Clinicians should consider Borrelia miyamotoi in patients with summer febrile illness—even when no tick bite is recalled.
Awareness of larval transmission may become increasingly important as emerging tick-borne infections continue to expand.
Related Articles
- Lyme Disease Co-Infections
- Can You Have Lyme Disease Without Seeing a Tick Bite?
- Where Is the FDA Test for Borrelia Miyamotoi?
- Lyme Disease Prevention Strategies
References
- Molloy PJ, Telford SR III, Chowdri HR, et al. Borrelia miyamotoi Disease in the Northeastern United States: A Case Series. Ann Intern Med. 2015;163(2):91-98.
- Krause PJ, Fish D, Narasimhan S, Barbour AG. Borrelia miyamotoi infection in nature and in humans. Clin Microbiol Infect. 2015;21(7):631-639.
Dr. Daniel Cameron, MD, MPH
Lyme disease clinician with over 30 years of experience and past president of ILADS.
Symptoms • Testing • Coinfections • Recovery • Pediatric • Prevention



I had 2 reddish itchy pimple rise up quickly in different locations (soft skin) each had a black spot into middle. I removed carefully each one. Under a jewelers eyeglass I saw legs attached to each black dots. The area small areas remained red. Pitched for a day. Deer tick nymphs? Christine Mancini Pgh PA 412-580-2439
You might consider sending in what you found to a professional like https://www.tickreport.com/.