Lyme Disease Statistics: Long-Term Symptoms, Missed Diagnoses, and Treatment Challenges
Lyme disease statistics highlight a troubling reality—many patients remain ill despite diagnosis and treatment. These infographic findings summarize key data from peer-reviewed studies on long-term outcomes, diagnostic limitations, and treatment response. :contentReference[oaicite:0]{index=0}
Patients may experience persistent symptoms when Lyme disease is not diagnosed early or treated adequately. In addition, diagnostic testing remains unreliable, and many patients never recall a tick bite or rash.
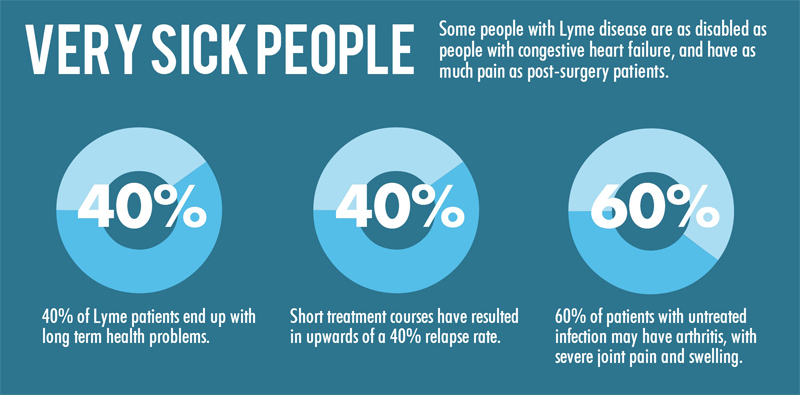
40% of Patients Develop Long-Term Health Problems
Long-term complications are common in Lyme disease:
- 34% of patients experienced arthritis, neurocognitive impairment, or neuropathy an average of 6 years after treatment
- 62% of patients reported persistent symptoms such as joint pain, fatigue, or neurologic involvement after 3.2 years
- At 6 months:
- 45% reported neurocognitive difficulties
- 36% reported new-onset fatigue
- 20% experienced widespread pain
These findings demonstrate that long-term symptoms are not uncommon—and may persist for years.
Short Treatment Courses May Lead to Relapse
Data from ILADS treatment guidelines reveal significant treatment failure rates:
- 38.5% failure with 20 days of cefuroxime
- 33% failure with up to 19 days of doxycycline
- 22.8% failure with up to 10 days of azithromycin
- 15.4% failure with penicillin or amoxicillin
In these analyses, treatment “success” required complete resolution of symptoms without relapse.
Even under strict definitions, a substantial proportion of patients did not achieve full recovery.
Untreated Infection Can Lead to Arthritis
In untreated Lyme disease:
- More than 50–60% of patients developed arthritis
- Symptoms included severe joint pain and swelling, often affecting large joints
- Onset ranged from days to 2 years after initial infection
This highlights the importance of early diagnosis and treatment.
Many Patients Do Not Recall a Tick Bite or Rash
Contrary to common belief:
- Only 37% of chronic neurologic Lyme patients recalled a tick bite
- Only 33% of Lyme encephalopathy patients reported a tick bite
Similarly, many patients do not recall a rash:
- 25% in early Lyme reports
- 39% in NIH trials (Krupp)
- 54% in NIH trials (Fallon)
Absence of a tick bite or rash does not rule out Lyme disease.
Diagnostic Testing May Miss Many Cases
The commonly used ELISA test has significant limitations:
- Only 37% of culture-confirmed Lyme patients tested positive
- Up to 63% of cases may be missed
This underscores the limitations of current diagnostic tools and the importance of clinical judgment.
Clinical Perspective
Lyme disease is a complex, multisystem illness with variable presentations and outcomes.
These data highlight three critical challenges:
- Delayed or missed diagnosis
- Limitations of current testing methods
- Incomplete response to standard treatment
Clinicians should consider Lyme disease even in the absence of a known tick bite or rash and recognize that persistent symptoms may reflect ongoing or inadequately treated disease.
Improved diagnostics, earlier recognition, and individualized treatment approaches are essential to improving patient outcomes.
References
- Shadick NA et al. Ann Intern Med, 1994.
- Asch ES et al. J Rheumatol, 1994.
- Aucott JN et al. Qual Life Res, 2013.
- Cameron DJ et al. Expert Rev Anti Infect Ther, 2014.
- Steere AC et al. Ann Intern Med, 1987.
- Logigian EL et al. N Engl J Med, 1990.
- Logigian EL et al. J Infect Dis, 1999.
- Steere AC et al. Arthritis Rheum, 1977.
- Krupp LB et al. Neurology, 2003.
- Fallon BA et al. Neurology, 2008.
- Nowakowski J et al. Am J Med, 2003.
Dr. Daniel Cameron, MD, MPH
Lyme disease clinician with over 30 years of experience and past president of ILADS.
Symptoms • Testing • Coinfections • Recovery • Pediatric • Prevention