Call for your appointment today 914-666-4665 | Mt. Kisco, New York
by Daniel J. Cameron, MD MPH
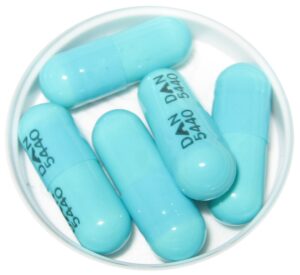
Study examines doxycycline as cause of acute pancreatitis in patient initially treated for suspected Lyme disease.
A 51-year-old man was admitted to the hospital with a one-week history of extreme fatigue, malaise, and confusion. Three days prior to admittance, the man had started oral doxycycline for presumed Lyme disease (LD). There were no reports of tick bites, high risk behaviors for contracting LD, or objective evidence of the disease. [1]
Upon further testing, the patient was diagnosed with acute pancreatitis. His labs revealed a lipase concentration of 5410 units/L (normal range, 13—60 units/L), an amylase concentration of 1304 (normal range, 28—100 units/L). A computed tomography (CT) scan of the abdomen showed mild stranding in the surrounding fat near the head of the pancreas, wall thickening of the duodenum, but no encapsulated fluid collection. [1]
The study published in the March 2016 issue of the American Journal of Health-System Pharmacy concluded that doxycycline was the probable cause of the man’s acute pancreatitis. Moy and colleagues, from the University of Connecticut Health Center, Department of Medicine came to this conclusion despite their admission that “Drug-induced pancreatitis is a diagnosis of exclusion; other etiologies of pancreatitis should be ruled out before concluding that drugs are the cause.”
The authors did not rule out other well-known etiologies of acute pancreatitis. The man presented with poorly controlled diabetes with a HA1C of 15 (normal, <5.7%), a blood sugar of 11,161 mg/dL (normal, 65—91 mg/dL), acidosis with a ph of 7.12, serum osmolality of 420 mOsm/kg (normal, 285—295 mOsm/kg), and renal failure with a creatinine concentration of 4.6 mg/dL (normal, 0.5—1.3 mg/dL).
The man rapidly improved with standard treatment for diabetic ketoacidosis. He was intubated, started on vasopressor support; received aggressive fluid resuscitation, hemodialysis and an insulin infusion.
Diabetes and DKA are also well-described causes of acute pancreatitis. Acute pancreatitis has been associated with Type 2 diabetes [2] and diabetic ketoacidosis. [3]
Doxycycline would be a reasonable treatment for a 51-year-old man who presented with a one-week history of extreme fatigue, malaise, and confusion. LD complications include Lyme encephalopathy, [4] chronic neurologic LD, [5] neuropsychiatric LD, [6] and post-treatment LD. [7]
The case report reminds us of the need to follow up with patients. The International Lyme and Associated Diseases Society‘s (ILADS) evidence-based guidelines discusses the need for reassessment. For example, Recommendation 3C states, “Clinicians should re-assess patients immediately following the completion of the initial course of retreatment to evaluate the effectiveness of retreatment and the need for therapeutic adjustments.” The guideline points out “Reassessment may need to be done much earlier and with greater scrutiny in patients with severe disease or when the therapeutic intervention carries substantial risk.”
There are side effects of doxycycline including photosensitivity and c. difficile. Typically, acute pancreatitis is not one of them. This patient’s illness was not caused by a 3-day course of doxycycline. In fact, the case study could only find two reports of doxycycline causing acute pancreatitis.
References
- Moy BT, Kapila N. Probable doxycycline-induced acute pancreatitis. Am J Health Syst Pharm, 73(5), 286-291 (2016).
- Gonzalez-Perez A, Schlienger RG, Rodriguez LA. Acute pancreatitis in association with type 2 diabetes and antidiabetic drugs: a population-based cohort study. Diabetes Care, 33(12), 2580-2585 (2010).
- Nair S, Yadav D, Pitchumoni CS. Association of diabetic ketoacidosis and acute pancreatitis: observations in 100 consecutive episodes of DKA. Am J Gastroenterol, 95(10), 2795-2800 (2000).
- Logigian EL, Kaplan RF, Steere AC. Successful treatment of Lyme encephalopathy with intravenous ceftriaxone. J Infect Dis, 180(2), 377-383 (1999).
- Logigian EL, Kaplan RF, Steere AC. Chronic neurologic manifestations of Lyme disease. N Engl J Med, 323(21), 1438-1444 (1990).
- Fallon BA, Nields JA, Parsons B, Liebowitz MR, Klein DF. Psychiatric manifestations of Lyme borreliosis. J Clin Psychiatry, 54(7), 263-268 (1993).
- Aucott JN, Rebman AW, Crowder LA, Kortte KB. Post-treatment Lyme disease syndrome symptomatology and the impact on life functioning: is there something here? Qual Life Res, 22(1), 75-84 (2013).




I took Doxycycline Hyclate 100mg on 6/21/2016 for 10 days. July 1, 2016 I started having pain in my abdomen. The pain became worse. I couldn’t stand to eat or drink. On July 5th I was admitted into the hospital for sever pancreatitis. I thought I was going to die the pain was so bad. I do blame the Doxycycline Hyclate for the attack. I was in the hospital for 11 days. This was my third pancreatitic attack in a year. The first attack was due to antibiotics. In Jan 2015 after a staph infection from spinal surgery turned into osteomyelitis. I’m sure you know the treatment for osteomyelitis, lots of intravenous antibiotics and eventually orally. April 2015 I was readmited to the hospital for severe pancreatitis due to antibiotics. I guess the rest of my life, I will be praying to never need any type of antibiotics again.
Thanks for sharing you story. There are other antibiotics not related to doxycycline. Let’s hope you never need them.
Dr. Carmeron–
First, thank you for commenting on the study that linked doxycycline use with pancreatitis. I was hoping that someone with some medical authority would question that assertion that was based on very thin (nonexistent?) medical evidence.
Second, I wonder if it is possible that Lyme itself is causing problems with the pancreas. I do see that late Lyme’s evil third cousin, syphilis, is linked with pancreatitis in the medical literature.
I am glad to see that you shared your concern regarding the poor link of doxycycline and pancreatitis. I have not seen pancreatic problems in my practice
I was diagnosed with walking pneumonia, I am a type 2 diabetic, with the diabetes under control .I also have a sensitivity to most drugs. I requested to the urgent care physicians assistant that she prescrib a Z-pac as that in the past (more than 5 years ago) it worked for me and was well tolerated by my sensitive system. She insisted that her facilities protocol was to prescribe Doxycycline and it was essentially the same as the Z-pac. I was given a dosage of 2 per day for 7 days. It mostly cleared my pneumonia symptoms but really wore me down significantly. Less than 24 hours after taking my last dosage, I started experiencing stomach discomfort. Over the next several hours the pain level increased radically accompanied by significant stomach distentia. Early in the morning my wife took me to our local hospital’s ER where after testing it was discovered that I was suffering from acute pancreatitis. My GI doctor and I agree given my history that Doxycycline is the primary reason for the onset of the acute pancreatitis, and now I’m in the middle of a painful and expensive 3 day hospital stay. Doctors, researchers and clinicians should make effort to seriously investigate this link and to warn patients of the real danger of taking this drug.
I am sorry to hear you suffered from acute pancreatitis. I have not seen pancreatitis due to doxycycline in my practice. The blog was referring to a case where pancreatitis was thought to be related to doxycycline. Instead, it was more likely to be due to poorly controlled diabetes, a common cause of pancreatitis. Thanks for sharing.
Yes something to say. I’m a 40 year old male, who suffered a pancreatic episode on 2016 due to gallstones and had it removed back then, end of the story.
2 years after ended in the er with a diagnosis of acute bronchitis and a viral infection, something the doctor labeled since he couldn’t figure out.
Treated and sent home with a Rx for doxycycline 100mg twice a day. On day four returned to the er with acute abdominal pain, vomiting and overall weakness. Trying to connect the dots find out that one of the possible side effects of the antibiotic was pancreatitis, and indeed was having acute pancreatitis that turned chronic.
Till today still suffering with symptoms of the pancreatitis like abdominal pain that radiates to the liver area and my back close to the kidneys area.
Hopefully will never have to take any antibiotics for any reason, and if I have to would go with one that already tried before, like the traditional one good ol penicillin. Hopefully they banned that specific one due to the high risk for pancreatitis.
Sorry to hear you had problems with pancreatitis. The case discussed was a complication of diabetes rather than pancreatitis.
Hi Dr. Daniel Cameron,
Have you heard of any patients that were treated for Lyme disease on Doxy that later developed Type 1 Diabetes? This happened to me. I was a healthy active 29 year old and got Lyme. then 4 years later was dx with Type 1 Diabetes. I was on a cycle of Doxy to treat the Lyme disease. I have always thought that the two were related some how.
Thank you for any insight you have on this.
I have not seen Type 1 diabetes develop after Lyme disease. They are both common conditions.
I was on Doxycyline in January 2019 for pneumonia. After taking this medication and finishing it. The next day I was sick as a dog and thought I was dying. I was admitted in the hopsital for 5 days. I was diagnosed with Pancreatitis due to this medication. I wouldn’t advise anyone to take this drug. Not only was I sick from it, I lost a whole month of work and seeing a specialist once a week and mulitple Cat scans. DO NOT TAKE DOXYCYCLINE!!
I’m a 34 year old male with lyme and Doxycycline if 100% responsible for my inflamed pancreatitis it really makes ur stomach hurt , when i paused taking it, all that stopped. Restarted and again the same thing happened. It is 100% a side effect. Other then that im healthy.
Thanks for your comments. The authors of the article I reviewed jumped to the conclusion that the pancreatitis was due to doxycycline. The blog reminded the reader that the pancreatitis was more likely due to the patient’s Type II diabetes and diabetic ketoacidoosis, both well-described causes of acute pancreatitis. That does not negate the possibility of doxycycline as an infrequent cause of pancreatitis. I have not seen pancreatitis due to doxycycline in my practice but I have seen pancreatitis due to other causes.
Interestingly, so many people take this medication and then present with acute pain in the abdomen several days after. My daughter is as admitted last night, second time in a year now, for this exact event. Does she have pre-existing stomach problems? Yes. She has been unable to tolerate NSAIDS and has general gastritis, undetermined cause, flares up. Non-celiac. Has this pattern of feeling like she is going to die 3-5 days post doxycycline happened twice in one year. Yes. Exactly so. She does not have Lyme disease. She was tested twice for this over the last five years. She is now in the hospital.
I have patients who cannot tolerate doxycycline even when taking it with food, probiotics and medications to control acids. In some cases, I have had to prescribe an antibiotic not related to doxycycline.
I absolutely have a documented case of drug induced acute pancreatitis (without necrosis) caused by doxycycline, I’ve never been treated for lyme disease and would be happy to share my records with you for research.
The blog refers to a published case of someone whose pancreatitis was more likely due to diabetic acidosis. The authors were only able to find two cases in the literature where pancreatitis was related to doxycycline. Thanks for sharing your case.