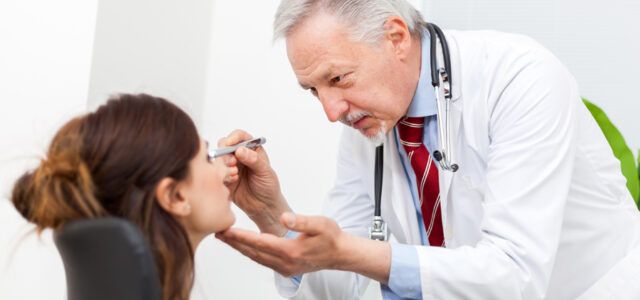
Lyme Disease Uveitis: Steroid Resistance and Diagnostic Clues
Lyme disease uveitis may be underrecognized and should be considered in patients with unexplained, steroid-resistant eye inflammation.
A retrospective study of 430 patients with uveitis identified seven cases of Lyme-associated uveitis. All seven patients showed steroid resistance but responded rapidly to antibiotic treatment.
The study included patients referred between 2003 and 2016. Six of the seven individuals had reported forest exposure, and two recalled a tick bite.
Clinical Presentation of Lyme Disease Uveitis
One patient had a history of erythema migrans, while others developed systemic features including arthritis, borrelial lymphocytoma, and lymphocytic meningitis.
These findings highlight the importance of evaluating Lyme disease symptoms beyond ocular complaints.
PCR testing was negative in spinal fluid for all seven patients, and four were negative on ocular testing, underscoring the diagnostic challenges of Lyme disease.
Steroid Resistance as a Key Diagnostic Clue
All seven cases of Lyme disease uveitis were resistant to corticosteroids, whether administered orally, topically, or via injection.
In contrast, all patients responded rapidly to antibiotics. Six were treated with intravenous ceftriaxone, and one received oral doxycycline.
This pattern—steroid resistance with antibiotic responsiveness—may help distinguish infectious uveitis from autoimmune causes.
Positive Serology Does Not Always Confirm Diagnosis
An additional group of patients tested positive for Lyme disease but were not classified as having Lyme-associated uveitis.
Some responded to steroids alone, while others had alternative diagnoses such as sarcoidosis.
This demonstrates that positive serology must be interpreted in clinical context and does not alone establish causation.
Diagnostic Considerations
The authors recommend considering Lyme disease uveitis when the following are present:
- Exposure history (tick bites, forest activity)
- Systemic findings such as rash, arthritis, or neurologic symptoms
- Steroid-resistant inflammation
These factors together improve diagnostic accuracy.
Frequently Asked Questions
What is uveitis in Lyme disease?
Uveitis is inflammation of the eye’s uveal tract that can occur with ocular Lyme disease. Symptoms include pain, redness, light sensitivity, and blurred vision.
How is Lyme disease uveitis different from other causes?
It is often resistant to steroids but responds to antibiotic therapy, which can help distinguish it from autoimmune uveitis.
Can PCR testing confirm Lyme uveitis?
PCR testing is frequently negative, even in confirmed cases. Diagnosis relies on clinical findings and response to treatment.
How is Lyme disease uveitis treated?
Treatment typically includes intravenous ceftriaxone or oral doxycycline, depending on the clinical presentation.
Does positive Lyme serology confirm the diagnosis?
No. Positive serology must be interpreted alongside clinical findings, as it does not prove causation.
Clinical Perspective
Lyme disease uveitis should be considered in patients with unexplained, steroid-resistant inflammation, particularly when accompanied by systemic or neurologic findings.
Failure to recognize an infectious cause may delay effective treatment.
Clinicians should maintain awareness of coinfections and overlapping presentations when evaluating complex cases.
Clinical Takeaway
Lyme disease uveitis is characterized by steroid resistance and rapid response to antibiotics.
Accurate diagnosis requires careful clinical correlation, as laboratory testing alone may be insufficient.
Related Reading
- Ocular Lyme Disease
- Optic Neuritis in Lyme Disease
- Orbital Myositis in Lyme Disease
- Growing List of Eye Problems in Lyme Disease
References
- Bernard A, Kodjikian L, Abukhashabh A, et al. Diagnosis of Lyme-associated uveitis: value of serological testing in a tertiary centre. Br J Ophthalmol. 2018;102(3):369-372.
Dr. Daniel Cameron, MD, MPH
Lyme disease clinician with over 30 years of experience and past president of ILADS.
Symptoms • Testing • Coinfections • Recovery • Pediatric • Prevention


I have PTLDS that has affected r eye showing uveitis
And left knee with osteoarthritis and little cartilage left and severe pain, myalgia. Orthopedics wants to replace knee and 3 eye Doctor’s does not know what to do for constant pain and feeling like object in r eye and photosensitivity. Help
I have patients who were diagnosed with PTLDS whose illness resolved with treatment for a persistent infection. I advise my patients to work with their other doctors to assess for other diagnoses