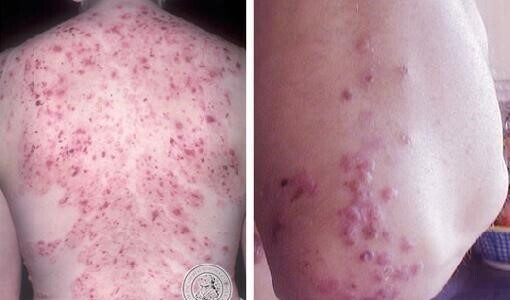
Can Lyme Disease Be Mistaken for Herpes or Shingles?
Some Lyme disease rashes may resemble herpes or shingles
Atypical skin findings can delay diagnosis and treatment
Disseminated Lyme disease may present with unusual rash patterns
Lyme disease is often associated with the classic bull’s-eye rash. But not all Lyme rashes follow the expected pattern.
Some patients develop atypical skin lesions that resemble herpes, shingles, cellulitis, insect bites, or allergic reactions. These unusual presentations may delay diagnosis and lead to inappropriate treatment.
A Lyme disease rash mistaken for herpes or shingles
In their article “Disseminated Lyme disease with a herpetiform center”, Zhang and colleagues described a woman in her 30s who developed a Lyme disease rash that resembled herpes lesions.
The patient initially developed a small red bump with surrounding swelling on her back, along with a rash in the left armpit and swollen lymph nodes.
She was prescribed cephalexin for presumed cellulitis. However, the lesions became larger, warmer, and more painful over time.
Skin examination later revealed a large circular erythematous plaque with a central cluster of vesicles and bullae resembling herpes infection.
Because some Lyme disease rashes may blister, burn, or appear in clustered patterns, they can occasionally resemble herpes zoster (shingles), particularly when lesions develop near the trunk or armpit region.
Disseminated Lyme disease may present with atypical rashes
The patient also developed additional erythematous patches on the breast and chest consistent with disseminated Lyme disease.
The authors ultimately diagnosed vesiculobullous erythema migrans associated with early disseminated Lyme disease.
She completed doxycycline treatment with full resolution of symptoms.
A Lyme antibody screen performed 6 weeks later was positive and confirmed by Western blot testing.
Learn more about Lyme disease symptoms and delayed Lyme disease diagnosis.
Why Lyme rashes are sometimes misdiagnosed
Classic erythema migrans with central clearing is easier to recognize clinically. But atypical Lyme rashes may present with:
- blistering or vesicles
- necrotic centers
- hemorrhagic crusting
- diffuse redness
- pain or burning
- multiple disseminated lesions
Atypical Lyme disease rashes are sometimes mistaken for cellulitis, shingles, herpes simplex, spider bites, fungal infections, or allergic skin reactions.
Because these rashes resemble herpes zoster, cellulitis, insect bites, fungal infections, or allergic reactions, Lyme disease may not initially be considered.
The authors noted that vesiculobullous Lyme disease may be more common than previously recognized.
Jarisch-Herxheimer reaction after treatment
The case also demonstrated a Jarisch-Herxheimer reaction after initiation of doxycycline therapy.
A Herxheimer reaction may temporarily worsen inflammation and symptoms after treatment begins, particularly in disseminated infections.
Learn more about Jarisch-Herxheimer reactions in Lyme disease.
Frequently Asked Questions
Can Lyme disease look like herpes?
Yes. Some atypical Lyme disease rashes may resemble herpes or shingles because of blistering, vesicles, or painful skin lesions.
Can Lyme disease be mistaken for shingles?
Yes. Vesiculobullous Lyme rashes may mimic shingles or herpes zoster, particularly when lesions are painful or blistering.
What is vesiculobullous Lyme disease?
Vesiculobullous Lyme disease refers to Lyme-associated skin lesions with blistering or bullae formation rather than the classic bull’s-eye appearance.
What is disseminated Lyme disease?
Disseminated Lyme disease occurs when infection spreads beyond the initial tick bite site and may involve multiple rashes, neurologic symptoms, cardiac findings, or systemic illness.
Can Lyme disease rashes be painful?
Yes. Although many erythema migrans rashes are painless, some atypical Lyme rashes may burn, itch, blister, or become painful.
Clinical Takeaway
Atypical Lyme disease rashes may resemble herpes, shingles, cellulitis, or other skin disorders, particularly during early disseminated infection.
Recognizing unusual Lyme rash presentations may help reduce delayed diagnosis and improve early treatment decisions.
Related Articles
These related articles explore atypical Lyme rashes, disseminated infection, skin manifestations, and diagnostic challenges.
Erythema Migrans Rash Doesn’t Always Have a Bull’s-Eye Appearance
Lyme Disease Skin Rash Puzzles Doctors, Leads to Misdiagnoses
What Does a Lyme Disease Rash Look Like?
Lyme Disease Misdiagnosis
Lyme Disease Symptoms Guide
References
- Zhang ZZ, Hashemi DA, Kroshinsky D. Disseminated Lyme disease with a herpetiform center. JAAD Case Rep. 2022;29:46-47.
Dr. Daniel Cameron, MD, MPH
Lyme disease clinician with over 30 years of experience and past president of ILADS.
Symptoms • Testing • Coinfections • Recovery • Pediatric • Prevention



My daughter went through this, but vaginal and buttocks. She was told it’s herpes and EBV . A couple of months later we finally found a specialist who diagnosed her with Lyme/Morgellons.
Diane,
bless you for continuing to look for the real cause.
This disease is mind boggling when we put all of our symptoms out there. Some of which can be embarrassing when it comes to look like an std. who wants to go tell a doctor that we have issues in this area but we know we’ve never done anything to cause. Seems like an unending problem.
I do wish for all who go through Lymes/coinfections to be healed in the Name of Jesus and lord please really soon
What an interesting case to highlight. Thank you.
Thanks. And thanks for your work.
Who was the specialist
Also looks like bacillary angiomatosis from bartonella spp
Good morning, Thank you so much for helping people all over the world with Lyme.
May you consider evaluating the sufferings of a teenager who is expected to undergo surgery soon to remove “under the arm skin complications”? She has suffered for years. She has been diagnosed with hidradenitis suppurativa which is a rare disease of which there is not a lot of information. She suffers pain, besides all the complications of numerous skin lesions, etc. physically, emotionally and mentally.
Is it possible that Lyme disease could be the underlying issue?
I know you cannot diagnose over the Internet, but any feedback will help.
I appreciate your expertise and support to the population dealing with Lyme disease. I have been diagnosed with Lyme disease – June 2021.
I have not seen a case of Hidradenitis suppurativa in my Lyme disease patients. Their painful skin condition would typically be followed by a dermatologist. I have had patients with Lyme disease that has been overlooked while being treated for another condition.
I was treated for Lyme for 10 days with Doxycycline Hyclate 100 MG CAP, two days after taking the last cap I got a tiny tick behind my knee. I developed a rash over practically my entire leg with little swelling, redness and itching worst than I can describe. Called my doctor and he said I was probably still protected from taking the meds ending two days ago, and did not need to see me. I called my GP again and they told me to go to Urgent Care if I was conserned and gave me an appointment for Tuesday, a week after calling them. I did go to UC because it was not getting better, it was red, swollen some and a rash that wouldn’t stop. At the UC I was prescribed Triamicinolone Acetinide Ointmrnt USO and 14 days Doxycycline Mono 100MC CAP. I was told to use the ointment and take the meds in 2 days if it doesn’t improve.The rash is not quite as bad after 1 day but the red around the bite still there, swelling gone down. I don’t know whether I should take the meds or not, as too much taking antibiotics can also cause problems. I still have an appointment with my GP in 3 days. This is rediculouse…..I know Lyme is in my system, will I ever get rid of it?
I am sorry to hear how complicated things have become. It typically use an individualized plan. I also consider Babesia, a coinfection