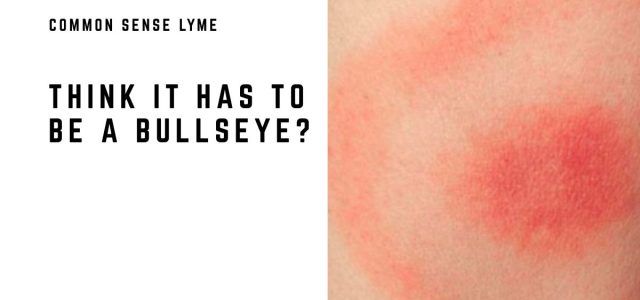
Lyme Disease Rash: What Does It Really Look Like?
Many people assume that a bull’s-eye or erythema migrans (EM) rash is a common manifestation of Lyme disease. And that the lack of a rash confirms a person does not have the disease. This is far from the truth.
EM rash identification remains a challenge because it often takes on a variety of appearances, according to a study by Burlina and colleagues.
“Only 20% of patients with an EM [rash] in the United States present with lesions that have the central clearing of a classic target lesion (‘ring-within-a-ring’ or ‘bull’s eye’).”¹
Instead, “the majority of EM lesions appear uniformly red or bluish-red in color and lack central clearing.”
Quick Answer: What Does a Lyme Disease Rash Look Like?
Only 20% of Lyme disease rashes present as the classic bull’s-eye pattern. Most appear as uniformly red or bluish-red patches without central clearing. Some look like cellulitis, others blister like shingles, and 20% of patients develop multiple rashes. Between 20-30% of Lyme patients never develop a rash at all, making it an unreliable diagnostic marker.
Why the Bull’s-Eye Rash Is a Myth
The classic bull’s-eye rash—a red ring with central clearing—appears in medical textbooks and public health materials as the defining feature of Lyme disease. But in clinical practice, only 1 in 5 patients present with this pattern.
This creates a dangerous misconception: patients and physicians assume that without a bull’s-eye rash, Lyme disease can be ruled out. The reality is that most Lyme rashes look nothing like the textbook image.
The majority of erythema migrans lesions appear as solid red or bluish-red patches without any central clearing. They may be round, oval, or irregular in shape. Some expand rapidly over days, while others remain relatively stable.
Lyme Rash Misdiagnosed as Cellulitis
Unfortunately, a Lyme disease rash may look like lesions found in other disorders. For instance, patients with Lyme disease may be misdiagnosed as having cellulitis. The treatment for cellulitis is not necessarily effective for Lyme disease.
Cellulitis typically presents with warmth, swelling, and tenderness—features that can overlap with erythema migrans. However, EM rashes are usually less painful and less warm to the touch than bacterial cellulitis.
When cellulitis is diagnosed and treated with antibiotics like Keflex (cephalexin), Lyme disease goes untreated because Keflex is not effective against Borrelia burgdorferi. This allows the infection to progress, potentially causing neurologic, cardiac, or joint complications weeks to months later.
Lyme Rash Misdiagnosed as Shingles
Between 4% and 8% of Lyme disease rashes present with central blistering. These cases can be misdiagnosed as shingles, a viral infection that causes blistering and is treated with anti-viral medications. Shingles treatment is not effective in treating Lyme disease.
Shingles (herpes zoster) typically follows a dermatomal distribution—appearing in a band along one side of the body. Erythema migrans with blistering may not follow this pattern and often expands over time rather than remaining confined to a nerve distribution.
When patients are treated with antivirals like Valtrex without considering Lyme disease, the bacterial infection continues unaddressed. By the time neurologic or systemic symptoms develop, the connection to the original rash is often lost.
Multiple Rashes: A Sign of Disseminated Lyme Disease
About 20% of patients have multiple EM rashes at the time of diagnosis due to the Lyme spirochete disseminating to other areas of the body. This presentation can be confused with erythema multiforme or other skin disorders.
Multiple rashes indicate that the infection has already spread through the bloodstream. These secondary lesions are typically smaller than the primary rash and appear days to weeks after the initial tick bite.
The presence of multiple rashes is a clinical indicator that early disseminated Lyme disease is present, often warranting more aggressive or prolonged antibiotic therapy.
Many Lyme Patients Never Develop a Rash
Perhaps most importantly, between 20% and 30% of Lyme disease patients never develop an erythema migrans rash at all. This means that absence of a rash cannot rule out Lyme disease.
Patients who present with fatigue, joint pain, cognitive dysfunction, or neurologic symptoms may have Lyme disease even without a visible rash. Relying on rash presence as a diagnostic requirement leads to widespread underdiagnosis.
Clinical Approach When Rash Is Uncertain
In practice, I treat with an antibiotic if there is uncertainty, as the consequences of missing a diagnosis of Lyme disease can be serious. If the rash is questionable, I often treat with antibiotics that would be effective for either Lyme disease or another possible condition.
For example, I might treat a patient with a rash that could be cellulitis or Lyme disease with an antibiotic that works for both such as cefuroxime rather than Keflex. I typically treat these cases longer if Lyme disease is a possibility.
Finally, I have also treated patients with a combination of an anti-viral medication (Valtrex) and cefuroxime if I am unsure whether the rash is related to shingles or Lyme disease. This dual approach addresses both possibilities while diagnostic clarity emerges.
Clinical Takeaway
Erythema migrans rash presents with highly variable appearances that defy the classic bull’s-eye description, creating diagnostic confusion and misdiagnosis as cellulitis, shingles, or other skin conditions when clinicians expect textbook presentations rather than recognizing the spectrum of Lyme rash manifestations. Critical diagnostic principles:
- Only 20% of Lyme rashes display classic bull’s-eye pattern—majority appear as uniformly red or bluish-red patches without central clearing, yet medical education and public health materials emphasize bull’s-eye appearance, creating false assumption that absence of target lesion excludes Lyme disease and contributing to diagnostic delays when patients and physicians dismiss non-classic presentations
- Lyme rash mimics cellulitis and shingles, leading to treatment with ineffective medications—4-8% of EM rashes blister centrally resembling shingles, while others present with warmth and redness suggesting cellulitis, resulting in antiviral or Keflex treatment that leaves Lyme infection unaddressed and allows progression to neurologic, cardiac, or joint involvement weeks later when connection to original rash is lost
- Multiple erythema migrans rashes indicate disseminated infection—20% of patients develop secondary lesions from hematogenous spread, appearing as smaller satellite rashes distant from tick bite site, signaling that infection has already disseminated and may warrant more aggressive or prolonged antibiotic therapy beyond standard early Lyme treatment protocols
- Twenty to thirty percent of Lyme patients never develop visible rash—absence of erythema migrans cannot exclude Lyme disease diagnosis, yet negative rash history is frequently used to dismiss clinical suspicion even when patients present with fatigue, arthritis, cognitive dysfunction, or neurologic symptoms in endemic areas with tick exposure, creating systematic underdiagnosis of Lyme disease in rash-negative cases
Frequently Asked Questions
What does a Lyme disease rash look like?
Most Lyme disease rashes appear as uniformly red or bluish-red patches without the classic bull’s-eye pattern. Only 20% have central clearing. Some look like cellulitis, others blister like shingles, and 20% of patients develop multiple rashes indicating disseminated infection.
Can you have Lyme disease without a rash?
Yes. Between 20-30% of Lyme disease patients never develop a visible rash. Absence of erythema migrans cannot rule out Lyme disease, particularly when patients present with systemic symptoms like fatigue, joint pain, or neurologic dysfunction in endemic areas.
How soon does a Lyme rash appear after a tick bite?
Erythema migrans typically appears 3-30 days after a tick bite, with an average of 7-14 days. The rash expands over days to weeks and may develop central clearing in some cases, though most remain uniformly colored.
Can a Lyme rash be mistaken for something else?
Yes. Lyme rashes are frequently misdiagnosed as cellulitis, shingles, spider bites, or allergic reactions. This leads to treatment with antibiotics or antivirals that don’t address Lyme disease, allowing the infection to progress untreated.
What does it mean if I have multiple Lyme rashes?
Multiple erythema migrans rashes indicate that Lyme disease has disseminated through the bloodstream to other areas of the body. This occurs in about 20% of cases and suggests more advanced infection that may require longer or more intensive antibiotic treatment.
Should I get tested for Lyme disease if I don’t have a rash?
Yes, if you have symptoms consistent with Lyme disease (fatigue, joint pain, neurologic symptoms) and tick exposure history. Standard two-tier testing has limitations, particularly in early infection, so clinical diagnosis based on symptoms and exposure remains essential even without a rash.
Related Reading
Rash and Misdiagnosis
- Lyme Rash Misdiagnosis: Not Always a Bull’s-Eye
- It Wasn’t Shingles. It Was Lyme Disease.
- Misdiagnosing Lyme Disease: The Great Imitator
Symptoms and Diagnosis
- Complete Guide to Lyme Disease Symptoms
- Understanding Lyme Disease Test Accuracy
- Early Lyme Diagnosis: Why Timing Matters
Treatment
References
- Burlina PM, Joshi NJ, Mathew PA, Paul W, Rebman AW, Aucott JN. AI-based detection of erythema migrans and disambiguation against other skin lesions. Comput Biol Med. 2020;125:103977.
- Steere AC, Strle F, Wormser GP, et al. Lyme borreliosis. Nat Rev Dis Primers. 2016;2:16090.
- Tibbles CD, Edlow JA. Does this patient have erythema migrans? JAMA. 2007;297(23):2617-2627.
Dr. Daniel Cameron, MD, MPH
Lyme disease clinician with over 30 years of experience and past president of ILADS.
Symptoms • Testing • Coinfections • Recovery • Pediatric • Prevention



I am glad you exist. I presented with an EM rash and a black legged tick at my GP, (an NP). She dismissed my concerns and said I had to wait for symptoms. I knew the rash is a symptom, so I tried several other practitioners, and Nurse practitioners, and all said the same thing. The NPs are used as gatekeepers in my Ivy league community in Western NY dominated by a callous hospital system with repeated write ups into the 2010s for keeping separate wing for poor people and gate keeping by labeling poor people as drug addicts to refuse care… It was over three years before I was able to get in front of a full fledged doctor, I presented him with all the info I had and your web URL, and he actually read it! At that point, I had inflammation and heat in my lower spine, and my left knee: he felt it was Lyme arthritis. He started antibiotic treatment, but I went into sepsis a week after the end of a medium course of doxicycline. It took another three years of constant on and off antibiotic cocktails until the symptoms of heat and pain stopped returning shortly after stopping the antibiotic treatment. Needless to say, I was nearly bed bound as my low back had locked up, adhesion in the low back fascia from lack of use, my discs were impinging on my spine according to a neurologist reading my MRI. I did have pre existing injuries to both my knee and low back, which complicated getting treatment as in NYS work related injuries are addressed as “off limits body parts” to deny care due to their choice, even though I was trying to get treatment for Lyme, they would refuse to examine me due to the body part, due to a pre existing work injury, the loophole they use to refuse care these days.
Regardless, it took another three years for the inflammation to resolve in my low back, just in time for my entire medical team to retire after COVID. 2023, over ten years after I first presented with a tick and rash for treatment, an MRI showed a gap between the formerly swollen discs and my cord, no impingement. I however have no intact discs in my lumbar, with the disc at the SI joint, a pre existing injury, now in pieces. I was able to start getting my legs back though, even though in 2023 I could only shuffle….