Lyme arthritis symptoms in young child emerge years after tick bite
Symptoms of Lyme disease may not present immediately following a tick bite. As this case report highlights, taking a thorough medical and travel history can be crucial in diagnosing and treating the illness.
Wheelchair-bound CEO regains ability to walk after Lyme disease treatment
Lyme arthritis is characterized by joint swelling lasting for weeks to months and potentially causing permanent joint damage. It can worsen symptoms in patients with existing joint conditions such as osteoarthritis and may go undiagnosed, leading to unnecessary surgeries.
Atypical Babesia symptoms in elderly man
Babesiosis is a tick-borne illness that can cause a wide variety of symptoms, making it difficult to diagnose. The number of cases in the U.S. has been rising – particularly concerning given that Babesia can be transmitted immediately following a tick bite or unknowingly through a tainted blood transfusion. Furthermore, this illness can be deadly or cause serious complications in immunocomprised patients.
Lyme disease can affect your eyes leading to various complications
Lyme disease has been associated with a broad range of visual problems including conjunctivitis, episcleritis, keratitis, uveitis, neuroretinitis, and retinal vasculitis. Patients with Lyme-related eye complications may experience blurred vision, eye pain or discomfort, visual floaters, double vision, eye flashes, red eye, headache, or sensitivity to light.
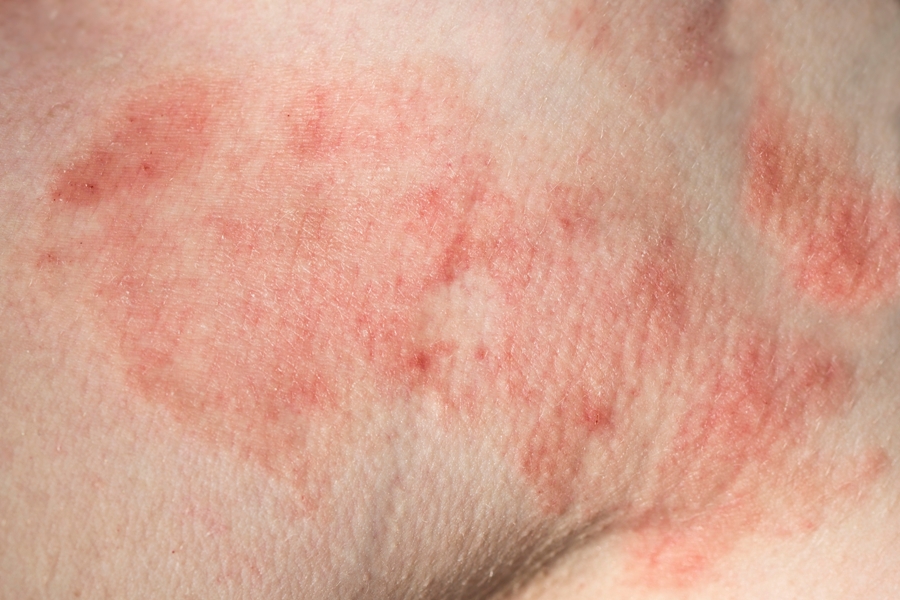
Lyme disease skin rash puzzles doctors, leads to misdiagnoses
Lyme disease can cause an atypical skin rash that may be mistakenly attributed to another illness, as this case report demonstrates. In their article, Suzuki and colleagues describe a 43-year-old woman who developed a rash which puzzled doctors and led to several misdiagnoses before Lyme disease was correctly identified.
Case report: Lyme neuroborreliosis with encephalitis
Investigators describe what they believe is the first case of confirmed Lyme neuroborreliosis encephalitis with significant parenchymal MRI changes in a broadly immunosuppressed patient.
Lyme disease causes mix of symptoms, including autonomic dysfunction
In the case report “A Patient with SIADH, Urinary Retention, Constipation, and Bell's Palsy following a Tick Bite,” Leone and colleagues describe a patient who developed an unusual combination of Lyme disease symptoms, all of which resolved following treatment. [1]
Woman develops Lyme disease symptoms after giving birth
In their article, “An Unusual Case of Serologically Confirmed Post-Partum Lyme Disease Following an Asymptomatic Borrelia burgdorferi Infection Acquired during Pregnancy and Lacking Vertical Transmission in Utero,” Pavia et al. describe the case of a young woman who developed symptoms of Lyme disease immediately following the birth of her child. [1]
How long does it take for a tick to transmit Babesia?
The numbers of cases of Babesia are climbing - a real concern, particularly since this tick-borne pathogen can be transmitted immediately following a tick bite. In their study “Lyme borreliosis: a review of data on transmission time after tick attachment,” Cook and colleagues describe the various timeframes it may take for an individual to become infected depending upon the tick-borne pathogen.
Atypical case of Lyme carditis in Florida woman
In this case report, “A Rare Presentation of Lyme Disease in an Immunocompromised Patient,” Basile and colleagues highlight atypical cardiac manifestations due to Lyme disease and the challenges in diagnosing Lyme carditis in immunocompromised patients. [1]