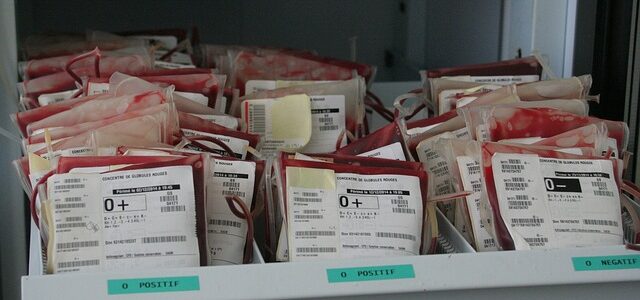
Premature Infants Contract Babesia From Blood Transfusions
Three premature infants contracted Babesia from a single blood donor.
The cases highlight challenges screening blood donors for babesiosis.
One infant relapsed more than a month after treatment.
A team of researchers at Yale School of Medicine describe three premature infants — all in one neonatal intensive care unit — who contracted Babesia from a single 24-year-old blood donor. The report was published in the Pediatric Infectious Diseases Journal. [1]
LISTEN TO PODCAST: Three premature babies who contract Babesia from blood transfusions
Babesia is a particularly frightening infection, given that it can be unknowingly transmitted to multiple people through blood banks, which have no foolproof way of screening donors.
“Screening questionnaires are clearly insufficient given the growing number of cases of transfusion-transmitted babesiosis,” writes Glanternik from the Division of Infectious Diseases, Department of Pediatrics at Yale School of Medicine.
Transfusion-transmitted babesiosis
The 24-year-old donor from Connecticut was not recognized by the blood bank and “was deemed suitable for donation by the American Red Cross and his serology was negative for all FDA-mandated tests,” Glanternik explains.
Three premature infants contracted Babesia from this donor, with two of the infants developing high-grade parasitemia (presence of parasites in the blood), according to Glanternik. The parasitemia rose to a high of 13.4% and 12.5% for Infant A and B, respectively. Parasitemia peaked at 6.8% for Infant C.
All three premature infants were treated with a combination of azithromycin and atovaquone despite published recommendations for clindamycin and quinine. [2] “The stability of oral suspension [of quinine] using capsules is undetermined,” explains Glanternik. “Furthermore, quinine’s narrow therapeutic index and potential adverse effects limits its utility in treating small children.”
The infants were treated for 14 days — longer than the 7-10 day recommendation described in the Infectious Diseases Society of America (IDSA) guidelines. [2]
However, more than a month (48 days) after treatment, one of the infants relapsed. There were no specific signs that could be attributed solely to babesiosis, explains Glanternik. But a “routine blood smear demonstrated relapse with 1% parasitemia.”
By day 9 of retreatment, the smear was negative. Treatment continued for a total of 23 days. None of the three premature infants required transfusions.
Authors warn of difficulties detecting Babesia in infants
“Clinicians should maintain a high index of suspicion for neonatal babesiosis in an infant who has received a transfusion because the clinical manifestations and concomitant lab abnormalities are non-specific and resemble those present in prematurity even in the absence of infection.”
Several additional questions are worth pursuing:
- Would longer initial treatment have prevented a relapse for Infant C.
- What are the consequences for infants if Babesia is not detected by thick smear?
- How can doctors be sure their newborns are clear of Babesia after clearing parasitology with Babesia by blood smear?
Related Articles:
Congenital transmission of babesiosis: two case reports
Transfusion-transmitted babesiosis popping up in more states in the USA
Sweats may be a sign of Babesia
Study raises concerns for Babesia patients and blood banks
References:
- Glanternik JR, Baine IL, Tormey CA, Rychalsky MR, Baltimore RS. A Cluster of Cases of Babesia Microti Among Neonates Traced to a Single Unit of Donor Blood. Pediatr Infect Dis J. 2017.
- Wormser GP, Dattwyler RJ, Shapiro ED, et al. The clinical assessment, treatment, and prevention of lyme disease, human granulocytic anaplasmosis, and babesiosis: clinical practice guidelines by the Infectious Diseases Society of America. Clin Infect Dis. 2006;43(9):1089-1134.
Dr. Daniel Cameron, MD, MPH
Lyme disease clinician with over 30 years of experience and past president of ILADS.
Symptoms • Testing • Coinfections • Recovery • Pediatric • Prevention



